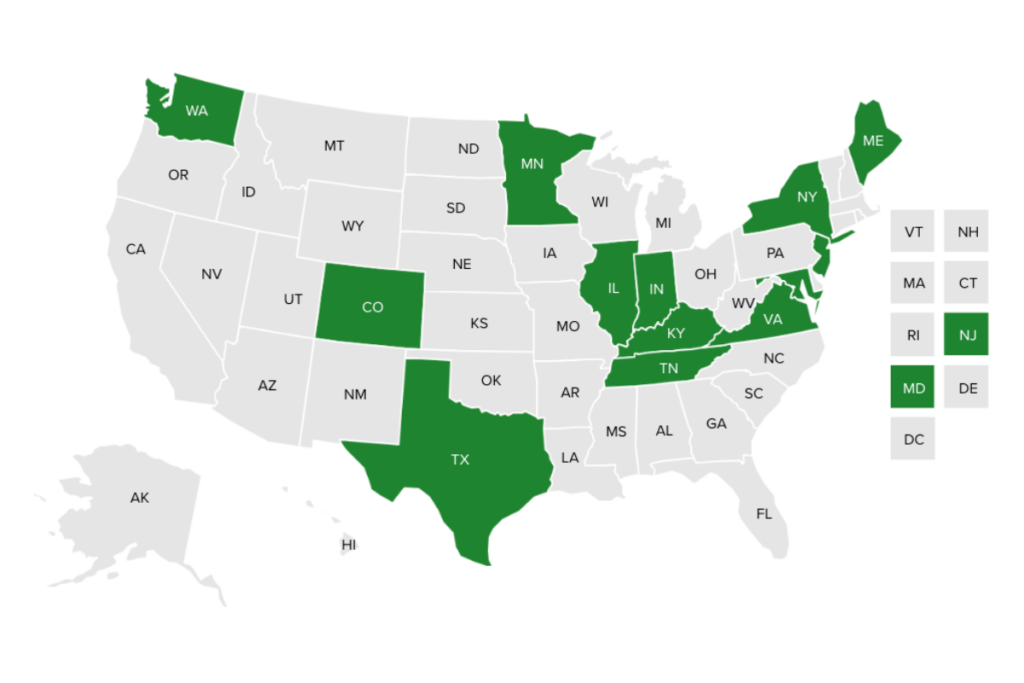
Access to maternity care is key to addressing the maternal mortality crisis. Midwife services can bridge gaps in health care, reduce health disparities, and support maternal and neonatal well-being.
This interactive map summarizes state Medicaid reimbursement policies for all types of midwives including certified nurse-midwives (CNMs) and midwives who pursue alternative pathways to licensure, often referred to as certified professional midwives (CPMs), certified midwives (CMs), or direct entry midwives depending on state regulations.
The accompanying tables provide a detailed description of individual state midwife policies, including licensure for some midwives. You can also download the charts on Certified Nurse-Midwife State Medicaid Reimbursement Policy and Midwife Licensing and State Medicaid Reimbursement Policy.
For questions or updates related to this research, please reach out to Dakota Staren at dstaren@nashp.org.
Definitions
For the purposes of this chart and map:
- Midwives refers to midwives without a nursing degree. Terminology for midwives without a nursing degree varies across states. Examples include: licensed midwives, direct entry midwives, certified professional midwives, and more.
- Certified nurse-midwives refers to midwives with a nursing degree.
Notes
*The information NASHP compiled about this state was not confirmed by the state’s Medicaid officials.
“N/A” indicates that information is not available for this state under this specific category.
“-” indicates that this information was not found for this specific category.
The Midwife Licensing and State Medicaid Reimbursement Policy table only includes states that provide Medicaid reimbursement for services performed by midwives (Certified Professional Midwives or Certified Midwives).
Acknowledgments
Emily Creveling, Anoosha Hasan, and Taylor Platt contributed to this publication through research. Carrie Hanlon and Karen VanLandeghem provided guidance and review. NASHP thanks the state Medicaid officials for their review. This 50-state analysis was made possible by the Health Resources and Services Administration (HRSA).